This story first appeared in the June 16, 2022 issue of our Good Grief! newsletter.
What is pharmacy’s role in improving palliative care? A vital one, according to those who know.
We’ve talked a lot in these pages about the need to improve access to palliative care and a 2022 survey shows that 96 per cent of Australians want to see it delivered more effectively in residential aged care facilities. These are the places where close to 30 per cent of Australians die.Yet currently only about one in 50 residents in aged care facilities receive palliative care.

This despite the fact that during the last four months of life, Palliative Care Australia estimates that 25 per cent of palliative care patients will have severe pain, and 60 per cent will have pain that causes them distress. Of course, elderly patients dying of old age don’t always die in great pain and sometimes it’s more like discomfort. But the pain and suffering of those in nursing homes is very poorly measured and addressed in this country, so how do we really know what their true needs are?
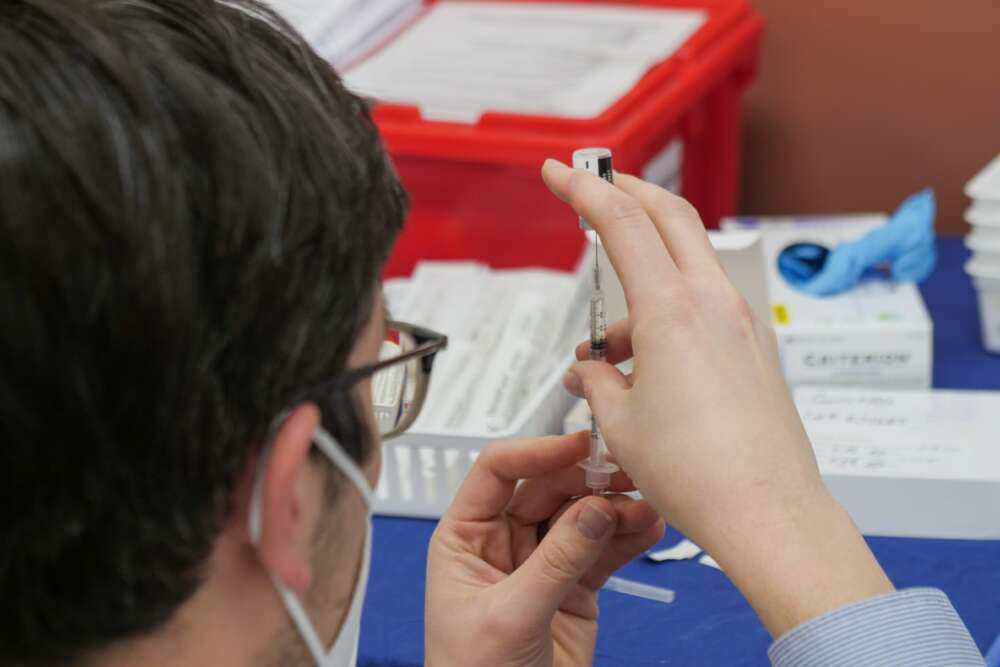
A key component of palliative care is to provide access to drugs which comfort and ease the pain and symptoms distinctive to dying.
Some people would prefer to die without medication, instead relying on other supports such as meditation. But this is not something that should be imposed by others. It is the choice of the dying. And to die pain free has been declared a basic human right by the World Health Organisation.
Six symptoms at the end of life.
NSW Health has identified six symptoms of the last days of life. These are:
- Pain
- Shortness of breath
- Nausea
- Anxiety
- Terminal restlessness
- Noisy breathing.
Good Grief! says any institution or group looking after the dying – whether that’s a hospital, private home or a nursing home (residential aged care facility) – should be able to provide relief from those six symptoms effectively and immediately.
Of these, maybe the least important is medication to stop noisy breathing – a polite but ineffective way of describing what historically is referred to as the ‘death rattle’, which occurs as mucous rolls across the throat making a resonating noise in the last hours of life. This doesn’t cause pain for the patient but can be extremely distressing for families and others supporting the dying person.
Addressing these six symptoms means accessing people with the qualifications, legal authority and wherewithal to provide the medicines needed.

Five drugs to deal with end-of-life symptoms
The five standard drugs delivered routinely today to prevent pain and discomfort at death are:
- morphine or other opioids – for pain and shortness of breath
- metoclopramide – for nausea
- clonazepam – for anxiety
- haloperidol – for terminal restlessness
- hyoscine butylbromide – for noisy breathing.
In NSW this list of five injectable drugs is called the “Core palliative care medicines.” They need to be injectable because the unconscious and/or close to death patient usually cannot take medication by mouth. There might be alternatives in each category, but these drugs are considered the most effective, most accessible and most affordable.
The NSW Clinical Excellence Commission recommends that community pharmacies (that is, those in your local shopping centre), should stock the five injectable medicines on the Core Palliative Care Medicines list. But this is only a recommendation and not mandated.
Across Australia, nursing homes have an enormous variety of arrangements for administering palliative care. And each of these variations have implications for speed of access – crucial when in the terminal phase is reached and medicine needs can change very quickly.

What are nursing homes doing about end-of-life pain relief right now?
We contacted five nursing homes in Sydney early in June, and found quite a variety of arrangements*.
On the Northern Beaches a nursing home there has one registered nurse on duty who can administer morphine and the other injections prescribed by one of the 13 doctors from the local area. Pharmaceuticals are delivered daily. But while this registered nurse is administering drugs routinely to all the other residents (usually with a bib on that says ‘Medications being administered, do not disturb’), what about those who have an emerging and sudden need?
At a Bondi nursing home palliative care is described as “available on site”. A registered nurse is on duty 24/7. A palliative care nurse visits daily and the local pharmacy provides the latest set of drugs in an early morning daily delivery. But what if the pain occurs at night or late afternoon?
But what if the pain occurs at night or late afternoon?
In Fairfield East at the home we rang there is no palliative care team on site, although palliative care is offered. The facility liaises with the Liverpool Hospital palliative care flying squad, a 12 minute drive late at night, and a 15 minute drive in the middle of the day. We know of cases where, adding the liaison between hospital and nursing home to this length of travel time, and the completion of consultations with other patients, this type of team can take more than an hour to arrive – and then they have to start making their assessment.
Also at that home, if a script needs to be made up, if the request is made early enough it will be delivered on the same day. But this is not promised. If an increase in morphine levels is required overnight, the patient will have to wait until morning.
Slightly further away, in a Liverpool nursing home, there are no registered nurses on duty overnight, despite the home being promoted as having 24/7 nursing and carer support. So, even if the doctor’s script says the dose is PRN – as needed, allowing for an increase in dose without a new script – an increase in the dose of morphine would have to wait until after the first registered nurse arrives on duty at 6am.
In contrast, inquiring about access to palliative care at a nursing home at Penrith, they explained that an after-hours doctor always comes when called, there is always the stock on hand to fill palliative care scripts and there is one registered nurse on duty overnight, two on in the morning and two in the afternoon.
*Thank you to Jenny Wilson for these interviews.
Clunky chains of command can be improved – Libby’s story.
We’ve heard and shared many stories of clunky chains of command failing patients in pain close to death in nursing homes. In one case, the family believed their mother Libby’s pain was worsening.
After raising this several times with the staff and being ignored, the family insisted the nursing home’s general practitioner was called. But he didn’t change Libby’s care plan. The lack of confidence of general practitioners to increase levels of pain relief is often reported, especially in those doctors who haven’t specialised in looking after the dying elderly. These are good examples of situations where an on-site or on-call pharmacist, specialising in the dying, could offer additional support.
The team from the local teaching hospital was contacted but explained they couldn’t come without a referral from the said general practitioner. Feeling they were trapped in a closed loop, the family rang the geriatrician who had seen Libby about three months before.
When he came the next day, he made the assessment that Libby – who had severe dementia and was non-verbal – had had a stroke. He prescribed morphine, writing the appropriate prescription and noting it was to be administered PRN. But the nursing home could only work with its standard pharmacy, which was out of stock. The morphine was not administered until 1pm the next day, 24 hours after his visit.
Her family believes Libby was in distressing levels of pain for at least a week before the first dose of morphine was administered.

The pharmacist’s capacity to help in nursing home care is underrated.
Pharmacy representatives say this situation would have been dramatically different if a pharmacist was on staff or was retained by the nursing home. The pharmacist could have liaised with the nurses and general practitioner much earlier in the week, and taken responsibility for ensuring that the medications needed were in stock, all steps which would have led to effective pain relief being delivered as soon as the pain was observed.
The pharmacist’s role in palliative care is incredibly underrated by everyone, often by pharmacists themselves, Kate Reed, Palliative Care Australia’s National Clinical Adviser told Australian Pharmacist in May last year.
It also needs to be recognised that the more drugs used for symptom management in palliative care, the greater the risk of adverse effects, and even though the person is dying, these are important complications of additional pain and suffering to avoid. Monitoring this is another role that a pharmacist with a special interest in palliative care can play.
The pharmacist’s role in palliative care is incredibly underrated by everyone, often by pharmacists themselves, Kate Reed, Palliative Care Australia’s National Clinical Adviser told Australian Pharmacist in May last year.
Ms Camilla Rowland, Chief Executive Officer, Palliative Care Australia told Good Grief!: “All Australians who are receiving palliative care, including people living in residential aged care facilities, must be able to access the medications they need to safely manage the pain and other symptoms related to their medical conditions,”
“People living in residential aged care with palliative care needs will often have multiple conditions requiring medications that treat both the underlying condition and symptom management, such as breathlessness. As a result, the choice, dose, route and appropriateness of these medicines will change quite regularly,” she said.
“We support approaches that optimise opioid management for people who will benefit. This means ensuring timely access to the appropriate opioids for pain and breathlessness management for aged care residents. This must be further supported by ensuring an adequate supply of commonly used opioids, and processes in place to manage planned or emergency shortages within aged care facilities.
“Residents may be left with poorly managed symptoms if qualified staff are not on-site to administer prescribed regular or breakthrough medication. Therefore, we support models of care that link palliative care teams, aged care facilities and local pharmacies working together to meet the needs of residents.”

Encouraging announcements by governments.
A spokesperson for the Pharmaceutical Society of Australia’s South Australia (SA) Branch explained: “SA Health is the largest provider of aged care beds in regional SA.”
This year, on March 25, the Australian government announced it was investing $345.7 million for on-site pharmacists and community pharmacy services in government-funded residential aged care facilities. This program will start on January 1, 2023.
This is as much to help with the other pharmaceutical needs of nursing home residents, outside their palliative care ones. But it will be a great step forward for those providing care to the dying.
On June 3 the South Australian government made a similar announcement. It’s $1.75 million pharmacy package for the state will include ‘embedding pharmacists in state-run aged care facilities’.

The Society argues: “All SA Health Aged Care sites should have access to an appropriately remunerated and accessible non-dispensing pharmacist.”
“The On-site pharmacists program is supported by key stakeholders including the Australian Medical Association (AMA), Leading Aged Services (LASA), Society of Hospital Pharmacists (SHPA) and Council of the Aging (COTA).”
It says residential aged care pharmacists will be able to identify, prevent and manage medication-related problems, ensure appropriate use of high-risk medicines including antipsychotics and opioids, help reach accreditation standards for medication management and educate facility staff, consulting GPs and other health professionals.
All of these are crucial to better management of the six distinct symptoms that occur at the end-of-life in nursing homes. And effective end-of-life management, despite our denials and delusions, should be at the core of good-aged care and it should be discussed in promotional materials given to those making inquiries about residing there. But maybe we are not ready for that yet.
Resources.

To find out more about the six symptoms and five medications referred to, go to:
https://www.health.nsw.gov.au/palliativecare/Pages/core-medicines-list.aspx
Palliative Care Australia’s then CEO Rohan Greenland said the organisation welcomed the inclusion of a new chapter on pain at the end of life in the 2nd edition of the Pain in Residential Aged Care Facilities: Management Strategies launched by the Australian Pain Society, in 2019. This was reported by Palliative Care Australia in 2019.
See Palliative care must become core business in aged care, 2020.
“Clearly articulated, robustly implemented. The Aged Care Quality Standards must include palliative care,” Palliative Care Australia, also said in 2020.
https://palliativecare.org.au/mediarelease/clearly-articulated-robustly-implemented-the-aged-care-quality-standards-must-include-palliative-care/
On-site pharmacists to improve medication management in RACFs.
https://www.health.gov.au/ministers/the-hon-greg-hunt-mp/media/on-site-pharmacists-to-improve-medication-management-in-racfs
Is death painful or more like uncomfortable?
https://good-grief.com.au/is-death-painful-or-more-like-uncomfortable/
Palliative Care: How pharmacists can help with medicines where needed, Australian Pharmacists, Vol 40, no 4, May 2021. https://www.australianpharmacist.com.au/palliative-care-how-pharmacists-can-help-with-medicines-where-needed/
Palliative Care Australia prepared a position statement in May 2019 Sustainable access to prescription opioids for use in palliative care which is directly relevant to the delivery of palliative care in nursing homes. It is endorsed by a number of organisations, including the Society of Hospital Pharmacists of Australia.
To read this important document, go to:
https://palliativecare.org.au//wp-content/uploads/dlm_uploads/2019/05/PalliativeCare-Opioid-Position-Final.pdf
In this statement Palliative Care Australia calls for eight key improvements to the delivery of palliative care, including: “Compulsory palliative care and opioid management education for all medical, nursing, allied health and pharmacists to be built into undergraduate curriculum to ensure a consistent baseline competency in pain and symptom management.”
This statement is supported by the organisations in the panel below.

