Gina has had some confronting news.
“I am a 62-year-old woman. I’ve been diagnosed with heart failure, (six months ago) and this will likely cause my death. At what point should I start seeing palliative care specialists? My cardiologist is coy about discussing this with me.”

The diagnosis took Gina completely by surprise because she is fit, trim and otherwise healthy. She is a passionate bike-rider, enjoys working with her husband on his farm and has recently retired from a very successful career in management.
While the practical advice from the cardiologist was good, Gina wanted more – she wanted to know how to prepare for the future, and to prepare her family realistically.
So, she organised her will. But she wanted more information, in lay person’s language, to help her shape her advance care plans and to be able to help her family understand her changing needs.

What is heart failure
Up to half a million Australians – and maybe even more – live with heart failure, says the Australian Institute of Health and Welfare. This is a terminal condition that shortens your lifespan, usually estimated up to about 10 years.
The latest Australian ABS figures show ischaemic heart disease – inadequate blood supply to the heart – was the leading cause of death in Australia in 2022.
Ischaemic heart disease is the cause of most heart failure and this occurs when your heart loses its capacity to pump blood around the body. In heart failure, the heart becomes enlarged.
The common symptoms of heart failure, documented by most heart health organisations, such as the Cleveland Clinic include:
- Breathlessness
- A sensation of difficulty breathing when lying down
- Waking up at night because of difficulty breathing
- Difficulty exercising
- Lethargy or low energy
- Tiredness and fatigue
- Swelling, caused by fluid retention, in the feet, legs and sometimes in the abdomen
- Dizziness
- Chest pain
- Coughing
- Heart palpitations
- Loss of appetite or nausea.
What the studies say
Heart failure is often caused by earlier heart problems. In a group of 153,592 people in a recent major Australian and New Zealand study, “Frequency, trends and institutional variation in 30-day all-cause mortality and unplanned readmissions following hospitalisation for heart failure in Australia and New Zealand. Eur J Heart Fail, 23: 31-40” high blood pressure (43 per cent), was the most common background heart problem which led to a person’s heart failure. Previous heart failure (36.6 per cent) and irregular heart-beat problems (20.1 per cent) were the next major causes.
But you could be like Gina, who’s heart failure is described as ‘idiopathic’, which means the cause is unknown.
The study mentioned above showed that 10.7 per cent of people diagnosed with heart failure died within 30 days of their first hospital admission, with 61 per cent of these deaths occurring while they were still in hospital. But that paints an unnecessarily alarming picture.
Put simply, survival rates decline with age.
Most people who die soon after diagnosis of heart failure are either extremely ill, often with their illness caused by another major disease or very elderly, and most people who present to the Emergency section of a hospital with the acute symptoms of heart failure are elderly.
Different impacts will cause the heart to lose the capacity to pump blood. So aside from the definition, of just ‘heart failure’, there is:
- congestive heart failure,
- left ventricular failure,
- right ventricular failure,
- hypertensive heart and kidney disease with congestive heart failure,
- hypertensive or heart and kidney disease with both congestive heart failure and kidney failure.
These are all different mechanisms that inevitably lead to the same outcome.
These are all different mechanisms that inevitably lead to the same outcome. The heart has two major chambers and they perform different functions. Damage to the left chamber of the heart means it can’t pump oxygenated blood to your body and damage to the right chamber means it can’t pump blood back into your heart to be re-oxygenated.
So, the causes are technically different but as the disease progresses, symptoms tend to become similar and left-sided heart failure often causes right-sided heart failure. Kidney failure is often associated with heart failure because damage to the kidneys will cause blood pressure to increase and this in turn places stress on the heart, further impairing the heart’s capacity to pump.
Chronic lung disease is also present in about 20 per cent of cases of heart failure, not surprising since the heart and lungs work so closely together.

The Good news
There’s actually a wide variation in survival and longevity of people first diagnosed with heart failure. It can be the subject of long papers explaining all sorts of statistics. Explains Maria Sheehan, nurse practitioner at the Heart Failure Service, St Vincent’s Hospital, Sydney: “Yes, you get a diagnosis, and there are high chances you may die within five years, if you have frequent hospital admissions…This is because the statistics show that there is a high mortality rate for a person within the first year if they have frequent admissions to hospital,” she says. “However, with good management many people do not end up having to go to hospital frequently and live quite a long time and what they consider a good quality of life. It’s very individualised.”
People don’t usually die suddenly from their heart failure, even if it develops quickly. It’s usually a slowly progressive condition. And because of a medical culture of early intervention, Australia has a good reputation for its success with helping people live a long and high-quality life with their heart failure.
That said, there are variations in the way it is managed in hospitals throughout the country with improvements in gaps and failures, the goal of public policy makers.
The story of Ed illustrates this.
Ed was diagnosed with heart failure. He went to a cardiologist with a good reputation for managing heart failure. But after a year of diagnosis and management, he was still quite breathless and didn’t appear to be any better. He had not been prescribed any medications, even though treating heart failure with medications is one of the greatest medical revolutions of the modern era.
This slows the progress of the disease and preserves quality of life, usually by helping the body excrete extra fluid. Ed couldn’t remember his blood pressure ever being taken by the cardiologist. He changed cardiologists. The new treatment offered was quite different. It involved more investigations, use of medications and more instruction on ways to manage his condition.
Within six months, his symptoms had vastly improved.
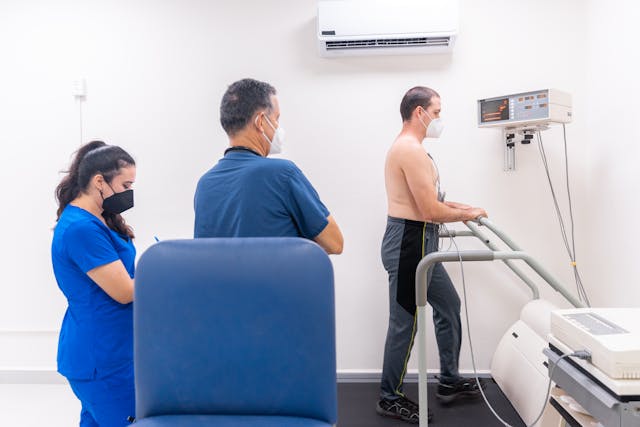
What happens as disease progresses?
There are two common pathways to diagnosis of heart failure. For some their diagnosis will be made by their primary health doctor – a general practitioner (GP) in Australia and the UK and a primary care physician in the USA, who has monitored, say, blood pressure and then noticed other changes.
In Australia, when your general practitioner suspects you have heart failure they will refer you to a heart specialist to confirm the diagnosis – your symptoms could be caused by something else.
What happens after diagnosis will depend on how severe your symptoms are. This could lead to a hospital visit or stay for further investigations and for monitoring including creating a ‘baseline’ of your symptoms, so that these can be compared at your next visit, and establishing you on medications, for example to help you lose excess fluids.
Here is the current “New York Heart Association’s Functional Classification” system for categorising heart failure, which is utilised around the world, including in Australia.
- Class I: No limitation of ordinary physical activity
- Class II: Slight limitation of ordinary physical activity – no symptoms at rest
- Class III: Marked limitation of ordinary physical activity – no symptoms at rest.
- Class IV: Symptoms on any physical activity or at rest.
The other path to diagnosis is an admission to hospital, often through the Emergency Department (also known as Accident and Emergency) when symptoms have appeared suddenly. Acute heart failure is one of the most common conditions presenting to emergency departments and patients often require hospitalisation. As mentioned before, these patients are usually elderly and have other heart conditions.
Even though currently just under a quarter of patients admitted to hospital for treatment will be readmitted within the first thirty days, the goal is to keep you well enough to stay out of hospital for as long as possible.

Management in the community
Community heart disease management programs, including for heart failure, have been developed to support people once they leave hospital and go back home. Their name and structure will vary slightly from one hospital to the next, but their goal is to keep you well and therefore reduce your chances of being readmitted to hospital.
You will play a big role in managing your disease, and you can do this from home. For example, since fluid retention both causes more damage to the heart and is a consequence of its lack of capacity to pump, a major goal will be to lower your fluid levels. This is the role of the medications you will be prescribed to take, and often you will be advised to limit your fluid intake, both actions that you can manage yourself.
Here is a list of lifestyle changes that can help improve your condition, from the American Heart Association’s Lifestyle Changes for Heart Failure.
- Monitoring your weight
- Quitting smoking
- Reducing alcohol intake
- Being physically active
- Getting enough rest
- Managing stress
- Eating for a healthy heart.
The cardiac team will work on these with you.

When will I die?
Hospitalisations because of heart failure have been declining since the 1990s, with more people surviving 30 days after their first hospital admission, and more people surviving beyond the first year. The explanation offered for this is better management strategies and better medications.
But when handed a diagnosis of heart failure, it’s reasonable to ask “When will I die?” and expect to be able to talk about this.
If you are worried about dying, whether within the next year, or even earlier, ask your cardiologist to discuss this with you.
But if they seem ‘coy’, to use Gina’s expression, you can ask them to refer you to someone who feels better able to talk about this.
Some cardiologists are not good at these discussions – something they often freely admit. Some believe they will serve you better if they remain optimistic and avoid the subject of death, even though not all patients want to be managed this way.
If you feel you are not able to discuss the subject with your cardiologist, make an appointment with your general practitioner to discuss this. Your general practitioner takes a ‘wholistic’ view of your health and should know your style when it comes to managing confronting information.
If they can’t work your concerns through with you, they can refer you to a psychologist.
You can also self-refer to see a psychologist. If you plan to do this, best to go through the Australian Psychology Association.
But in Australia, the benefit of going through your general practitioner is that they can offer you a ‘mental health’ plan, most of the cost of which can be recovered through Medicare. They are also familiar with best providers in your area and know those providers with a good reputation.
If you are working, employee assistance programs which provide free counselling through your workplace might also be helpful.
Another way of approaching your fears is to share your experience with others.
The Heart Foundation offers peer support through its My Heart, My Life program, which can be found at https://www.facebook.com/groups/myheartmylifecommunity

Long-term management of heart-failure
The cardiac management team will monitor and assess you, once your diagnosis is confirmed, with the expectation they will be advising you for several years.
“We look at how you present and how well you were doing, say, six months or a year ago,” explained Maria Sheehan.
“We look at how your heart is functioning, using objective tools such as ultrasound.
“One person’s cardiac ultrasound can show poor heart function, yet they have very few symptoms. Yet if you look at the ultrasound of another person, they may have the same poor heart function and have significant symptoms.
“Management of your symptoms will depend on a number of issues: how well you are, how many other conditions you’ve got, how old you are, how well you’ve looked after yourself, how much you take on the advice we give you, and if you take your medications.”
“This is about getting to know you at the beginning. We find out what your quality of life is like and then teach you what to do to manage your symptoms,” said Maria.
“And we say ‘If there’s any stage when you need more and things aren’t working for you, come back and we can discuss which way we need to go.’
“That deterioration might be in six-months’ time, in a year’s time or it might be in two years’ time. But whenever it is, the team is there for you.”
Remember, you’re not expected to manage heart failure on your own. If you’re feeling isolated or are struggling with it alone, you are not being connected with the right services, so discuss this with your general practitioner or someone who can advocate for you.

When you keep going back to hospital
You might be the person who can manage your symptoms extremely well, so doesn’t need to be admitted to hospital very often, and when you are, you have a short spike of illness before quickly bouncing back, although maybe not to quite the level of heart health you had before.
Unlike hospital admission patterns for cancer which have a long period of wellness followed by a sudden decline, with heart failure disease you have a slow, progressive decline. A sudden deterioration will be treated in hospital and then you will go home again and this pattern will be repeated often.
“You’re on a gradual downward trajectory over a period of time. You may have dips down where you have worsening heart failure symptoms for example, when you become fluid overloaded,” explains Maria.
“It’s about managing those dips so they are few and far between, aiming to prevent them altogether.”
About 40 per cent of re-admissions to hospital with heart failure are because a patient has lost their way with their own management. So it’s an opportunity to get help.
One of the community nursing team, popping in regularly to give advice, can recognise the problem and start treatment immediately.
End stage of heart failure and palliative care
When you reach end stage heart failure your life expectancy is reduced to around 6–12 months and your quality of life is poor.
Typical symptoms at this stage are pain, persistent cough, fatigue and breathlessness that substantially interfere with living.
It used to be thought that palliative care should only be offered at the end stage of heart failure but now it’s recognised that this support needs to come much earlier.
And it needs to be planned well before your symptoms reach end-stage. Palliative care can help with the psycho-social aspects of your well-being, not just the physical ones, for example, advance care planning and decision-making about treatment.
Details about this new way of thinking are well expressed in the 2018 Canadian article A palliative approach for heart-failure end-of-life care, by Jane Maciver, and Heather Ross.
The authors say that today the symptoms you experience are more important than any theoretical trajectories about how long you are expected to live. And the palliative care team should be involved early, ideally as part of your cardiac team, so care doesn’t become fragmented.
They point out that effective advance care planning improves quality of life, satisfaction with care, lowers rates of depression and anxiety amongst bereaved family members and lowers healthcare costs.
They also note that the approach to advance care planning in heart-failure has changed. Whereas in the past, a plan would be made early and then followed this has changed because “it is impossible to know the future context in which these decisions are made.”
Instead, the patient and their substitute decision maker are taught how to participate in complex decision making, with each new situation, as the medical situation worsens (link). The patient is seen as a partner with the medical team in this.
It doesn’t sound much on paper, but this is a radical shift, from the old approach, a “new paradigm” as the authors say.
This discussion is in line with today’s approach to palliative care. And other papers are looking at shifting the emphasis from prolonging life to ensuring quality of life.
Do you want to die at home? And what level of medical interventions do you want, knowing that your disease will not be cured? These are questions you are entitled to explore thoroughly.
Resources
- Is it time to see your GP to ask about your heart? For information about what such a health check entails, go to: https://www.heartfoundation.org.au/Heart-Health-Education/Heart-Health-Checks
- The Heart Foundation offers peer support through its My Heart, My Life program, which can be found at https://www.facebook.com/groups/myheartmylifecommunity
- There are other support programs too, for example, Heart Support Australia Ltd.
- To find a psychologist, go to the Australian Psychology Society’s Find a Psychologist page.
To read in depth on the new approach to palliative care for those with end stage heart failure, see:
- A palliative approach for heart failure end-of-life care. Maciver, Jane; Ross, Heather J. Current Opinion in Cardiology 33(2):p 202-207, March 2018.
To read an article that discusses improvements in symptom management, that shift the emphasis from prolonging life to ensuring quality of life, see:
- End-of-life care in patients with advanced heart failure. Diamant, Michael J.; Keshmiri, Hesam; Toma, Mustafa. Current Opinion in Cardiology 35(2):p 156-161, March 2020. | DOI: 10.1097/HCO.0000000000000712.
